Alagille syndrome is a rare, multisystem disease that largely affects the liver. It can also affect other major parts of the body, including the heart, face, eyes, kidneys, and spine.
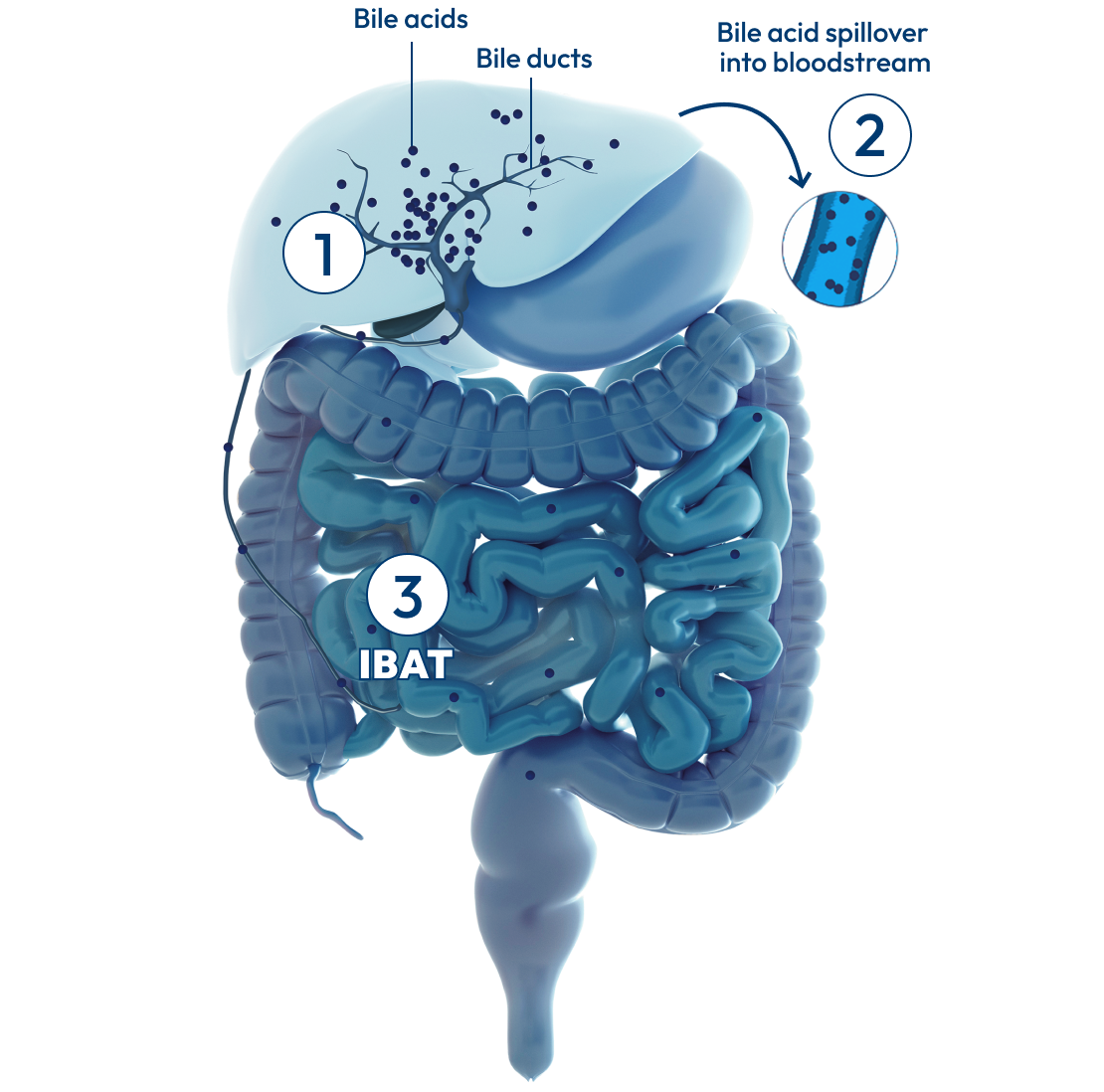
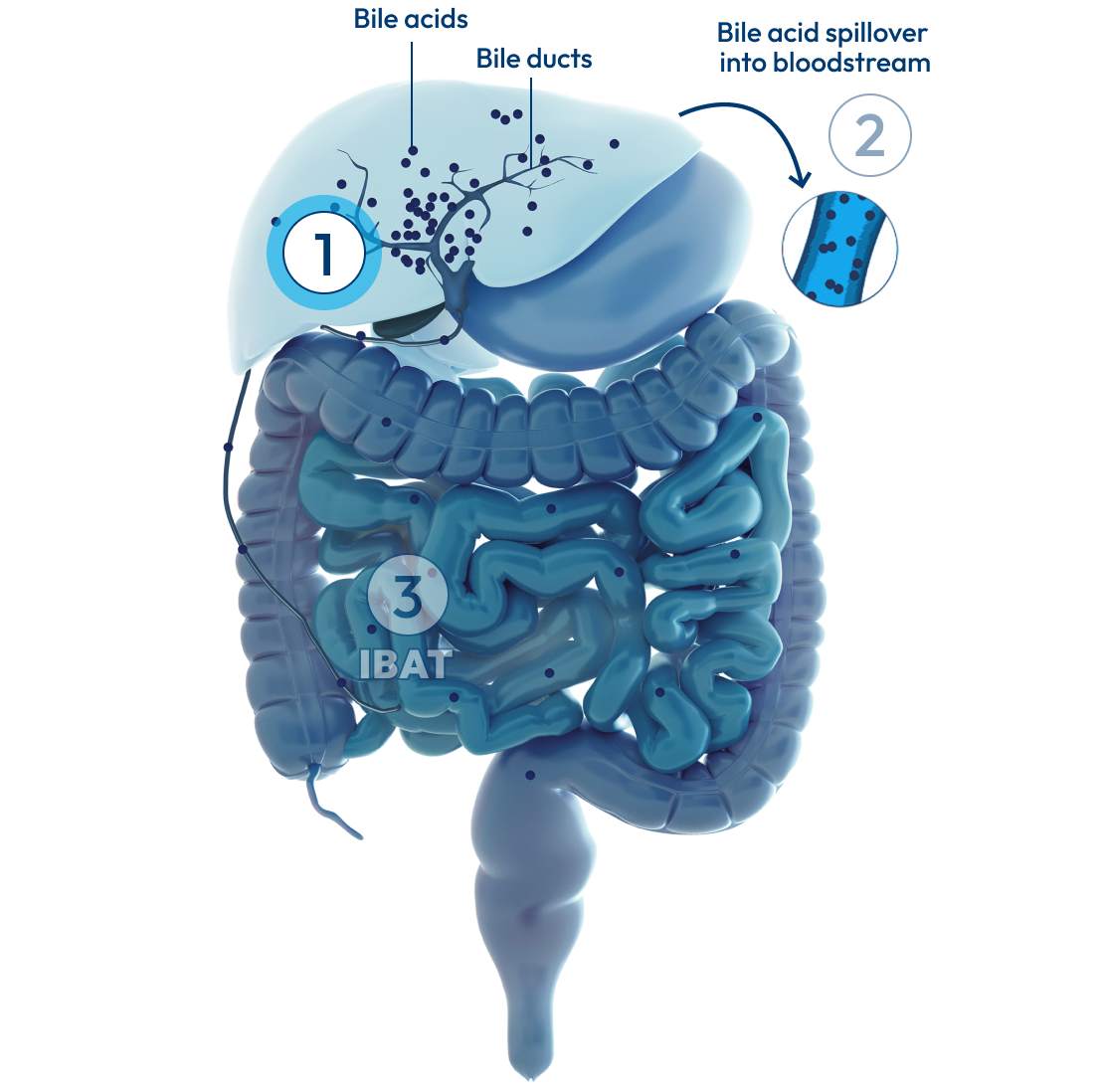
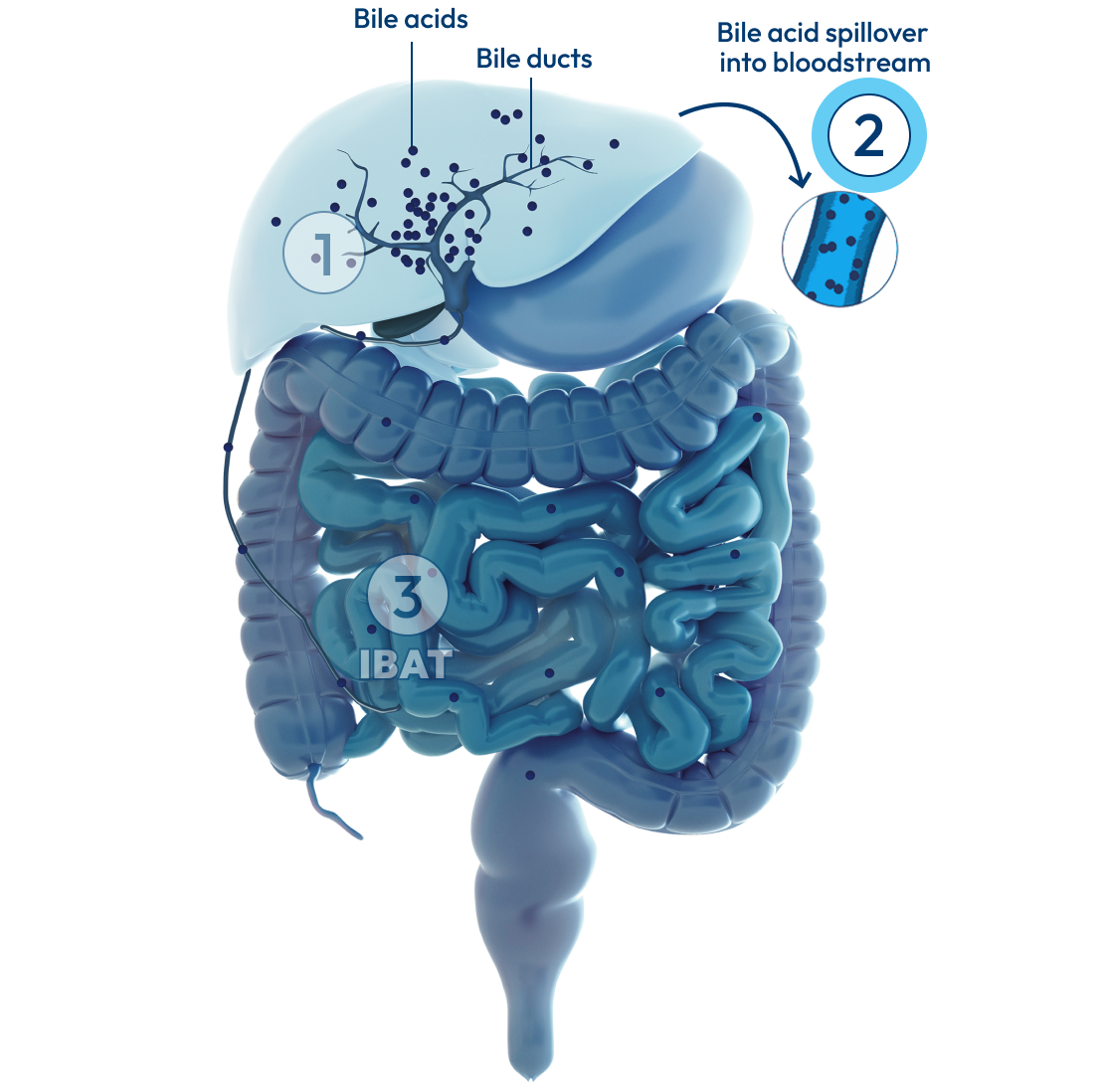
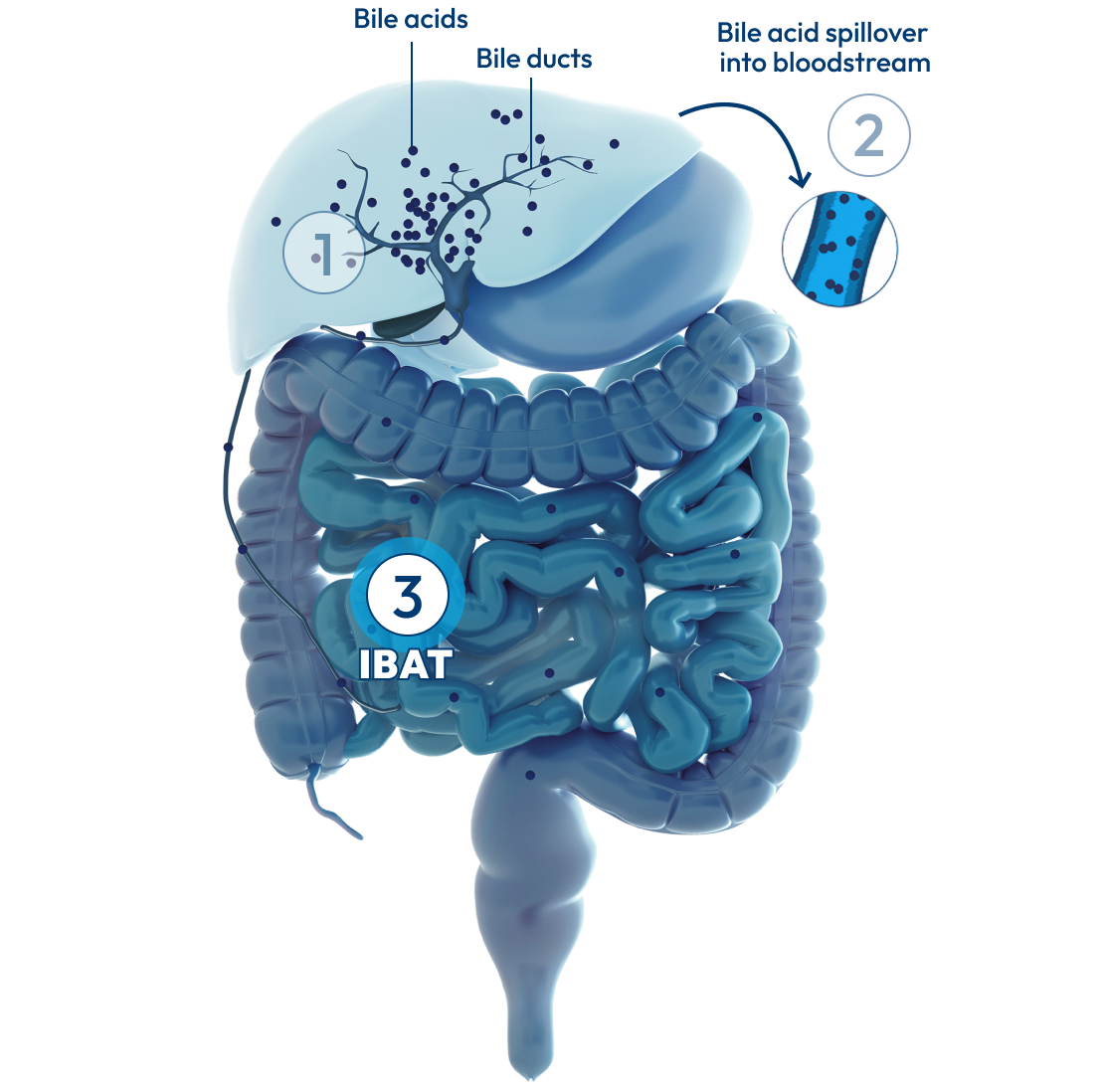
In people with Alagille syndrome, the bile ducts may be too narrow, too few, or missing altogether. This can result in cholestasis: a condition where the flow of bile from the liver is slowed or blocked, causing bile acids to build up in the body.
Over time, the buildup of bile acids in the liver can lead to long-term problems, including:
of people with ALGS are affected by cholestatic pruritus, and it is considered the most burdensome symptom.
Cholestatic pruritus is often a very challenging symptom for people with Alagille syndrome, beyond the scratching. It can be difficult to navigate the itch without the right support. Signs and symptoms related to the itch can look different during the day and/or night, vary among patients, or even change with age.
Cholestatic pruritus may only happen occasionally or may get worse during certain times of the year. Some people refer to times when cholestatic pruritus is worse as “flare-ups.”
Cholestatic pruritus can be mistaken for other common causes of itch, such as:
In the past, there were limited treatment options for cholestatic pruritus in Alagille syndrome. As a result, burdensome symptoms like the itch and the damage caused by bile acid buildup often led to surgery or liver transplant being used as treatment.
Persistent cholestatic pruritus was a reason in 49% and 82% of liver transplants in patients with Alagille syndrome.*†
- *A retrospective review assessing information of 163 children with Alagille syndrome and liver involvement between 1960 and 2000 found that among the 44 patients who received a liver transplant, refractory (persistent despite treatment) pruritus was a reason in 36 patients (82%); xanthomas (deposits of fat under the skin) that affect appearance were a reason in 32 patients (73%), bone fractures in 15 patients (34%); and/or signs of end-stage liver disease in 5 patients (11%).
- †A multicenter retrospective (looking back in time) study of 1433 children with Alagille syndrome assessed outcomes in 1184 of those children who presented with neonatal cholestasis. Among the 328 patients who received a liver transplant and had recorded reasons (some patients had more than 1 reason), intractable (persistent) pruritus was listed as a reason in 161 cases (49%). There were 235 cases of ≥1 complication of persistent cholestasis (72%); of these, growth failure was a reason in 127 cases (54%); xanthomas in 116 cases (49%); metabolic bone disease in 16 cases (7%); fat-soluble vitamin deficiency in 3 cases (1%).
—Michelle, mom to Téa, living with Alagille syndrome
Hear from Téa, who struggled for years with persistent itching and disrupted sleep.
Not all patients taking LIVMARLI and their caregivers will have the same experiences.
Michelle: I categorized her itch as mild, and I think because I just made it so—it was so normal, it was just a part of our life at that point that I regret it because it wasn’t normal. It was affecting her daily life. There was an opportunity for us to get into a trial with LIVMARLI. Téa wasn’t able to access the trial because I categorized her as mild. Hearing other people’s stories on their itching, I was like, “okay well, she’s not doing that. It’s not that bad, or if it’s cool in the home, she’s not itching that bad.” I always found something to be like, “okay, it’s not that bad,” but in reality it was.
All levels of cholestatic pruritus deserve attention. Check out LIVMARLI.com/between-the-fines to hear real people open up about their lives with cholestatic pruritus.
Take the itch quiz
The following questions can help you identify the signs and symptoms of cholestatic pruritus, the impact they have on your everyday life, and how well they're currently managed. No matter the outcome, be sure to share your quiz summary with your doctor.